|
How Can I Help Protect My Baby....
...during pregnancy? ...when my water breaks or I start labor? ...after my baby is born? |
(Click HERE to VIEW or DOWNLOAD the following in our brochure’s checklist format.)
Group B strep (GBS) is a type of bacteria that is naturally found in the digestive and lower reproductive tracts of both men and women. About 1 in 4 pregnant individuals "carry" or are "colonized" with GBS. Carrying GBS does not mean that you have an infection or are unclean. Anyone can carry GBS. However, invasive group B strep disease (iGBS) can occur when GBS causes an infection.
Unfortunately, babies can be infected by GBS before birth through several months of age due to their underdeveloped immune systems. Only a few babies who are exposed to GBS become infected, but GBS can cause miscarriage, stillbirth, preterm birth and infection in newborn babies possibly resulting in lifelong health challenges or even death. GBS most commonly causes infection in the blood (sepsis), the fluid and lining of the brain (meningitis), and the lungs (pneumonia). Some GBS survivors experience handicaps such as blindness, deafness, mental challenges, and/or cerebral palsy.
Fortunately, most GBS infections that develop at birth can be prevented if pregnant individuals who have tested positive receive at least 4 hours of IV antibiotics just prior to delivery.
Unfortunately, babies can be infected by GBS before birth through several months of age due to their underdeveloped immune systems. Only a few babies who are exposed to GBS become infected, but GBS can cause miscarriage, stillbirth, preterm birth and infection in newborn babies possibly resulting in lifelong health challenges or even death. GBS most commonly causes infection in the blood (sepsis), the fluid and lining of the brain (meningitis), and the lungs (pneumonia). Some GBS survivors experience handicaps such as blindness, deafness, mental challenges, and/or cerebral palsy.
Fortunately, most GBS infections that develop at birth can be prevented if pregnant individuals who have tested positive receive at least 4 hours of IV antibiotics just prior to delivery.
Although most people do not have any symptoms, GBS can cause vaginal burning, vaginal irritation and unusual discharge which may be mistaken for a yeast infection and treated incorrectly. (1) If you have vaginitis symptoms, see your healthcare provider promptly for an exam and possible GBS testing.
GBS can also cause bladder infections, with or without symptoms. Your provider should do a urine culture for GBS and other types of bacteria (this is not the standard prenatal urine “dipstick” check) at the first prenatal visit. GBS in your urine means that you are likely heavily colonized vaginally which puts your baby at greater risk.(2) If your urine tests positive, your provider should consider you to be GBS positive (GBS+) for this pregnancy so that you receive IV antibiotics for GBS when labor starts or your water breaks.
It is now the standard of care in many countries to be routinely test for GBS between 36 and 37 weeks of each pregnancy unless a urine culture is positive in the current pregnancy or a previous baby was infected by GBS. Testing is done by taking a swab of both your vagina and rectum. Your test result should be available in 2–3 days. Be aware that you may test negative for GBS (GBS-), but be GBS+ later and vice versa as GBS colonization can change. Ask your provider about being tested again if GBS- in a test done before 36 weeks.
GBS can also cause bladder infections, with or without symptoms. Your provider should do a urine culture for GBS and other types of bacteria (this is not the standard prenatal urine “dipstick” check) at the first prenatal visit. GBS in your urine means that you are likely heavily colonized vaginally which puts your baby at greater risk.(2) If your urine tests positive, your provider should consider you to be GBS positive (GBS+) for this pregnancy so that you receive IV antibiotics for GBS when labor starts or your water breaks.
It is now the standard of care in many countries to be routinely test for GBS between 36 and 37 weeks of each pregnancy unless a urine culture is positive in the current pregnancy or a previous baby was infected by GBS. Testing is done by taking a swab of both your vagina and rectum. Your test result should be available in 2–3 days. Be aware that you may test negative for GBS (GBS-), but be GBS+ later and vice versa as GBS colonization can change. Ask your provider about being tested again if GBS- in a test done before 36 weeks.
|
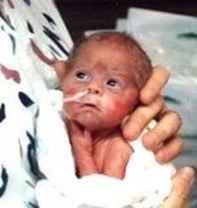
Carissa was born weighing 1 pound, 12 ounces because GBS caused her mother to go into preterm labor.
|
|
…during pregnancy?

Ask to have a urine culture for GBS and other types of bacteria done at your first prenatal visit.(3) If you have symptoms of a urinary tract infection (UTI) or a significant level of GBS in your urine, your healthcare provider should prescribe oral antibiotics at the time of diagnosis. (2) GBSI advocates a recheck (“test of cure”) one month after treatment.
See your provider promptly for any UTI and/or vaginitis symptoms.(4)
Be aware that bacteria can be passed between sexual partners, including through oral contact.(5)
Contact your provider immediately if you experience:
Get tested during your 36th or 37th week of pregnancy. Tell your healthcare provider if you are using antibiotics and/or vaginal medications which may cause false negative results. (7) (If you test negative, ask your healthcare provider about being tested again if you have not given birth within five weeks.)
Get a copy of your GBS results to keep with you!
Plan ahead if you have short labors or live far from the hospital.The IV antibiotics you receive in labor generally take 4 hours to be optimally effective.
Tell your provider if you are allergic to penicillin and describe your reaction. There are IV antibiotic alternatives if necessary.(2)
Know that “alternative medicine” treatments such as garlic or tea tree oil have not been proven to prevent your baby from becoming infected. Some treatments may be unsafe.
Wren’s mother followed an alternative regimen of acidophilus, echinacea, garlic capsules, vitamin C, grapefruit seed extract, and garlic suppositories to eradicate GBS from her body when pregnant with Wren. Wren was 7 pounds, 20.5 inches and perfect at birth after a normal labor and delivery at home. He died 11 hours later from a group B strep infection in his lungs.
Avoid unnecessary, frequent, or forceful internal exams which may push GBS closer to your baby. Knowing how far you are dilated does not accurately predict when your baby will be born.(8-10) Vaginal or perineal ultrasounds are less invasive options.(11,12)
Discuss the risks vs. benefits of possible methods of induction with your provider well before your due date as not all providers ask before “stripping” (also known as “sweeping”) membranes.
Ask your provider to not strip your membranes if you test positive for GBS. (Be aware that you may test negative, but be GBS+ later.) GBS can cross intact membranes and procedures such as stripping membranes and using cervical ripening gel to induce labor may push GBS as well as other bacteria closer to your baby.(13-16)
If you are having a planned C-section, talk to your provider about the potential risk of GBS infection and the risks vs. benefits of starting IV antibiotics for GBS well before your incision. IV antibiotics for GBS are not indicated per the US guidelines for a planned C-section done before your water breaks or labor starts as the risk of GBS infection in this situation is very low.
Talk to your provider about whether or not to use internal fetal monitors and/or have your water broken before you have had IV antibiotics for at least 4 hours.
See your provider promptly for any UTI and/or vaginitis symptoms.(4)
Be aware that bacteria can be passed between sexual partners, including through oral contact.(5)
Contact your provider immediately if you experience:
- Decreased or no fetal movement after your 20th week
- Frenzied or sudden excessive fetal movement (6)
- Any unexplained fever
- Any signs of preterm labor or your water breaks before your 37th week
Get tested during your 36th or 37th week of pregnancy. Tell your healthcare provider if you are using antibiotics and/or vaginal medications which may cause false negative results. (7) (If you test negative, ask your healthcare provider about being tested again if you have not given birth within five weeks.)
Get a copy of your GBS results to keep with you!
Plan ahead if you have short labors or live far from the hospital.The IV antibiotics you receive in labor generally take 4 hours to be optimally effective.
Tell your provider if you are allergic to penicillin and describe your reaction. There are IV antibiotic alternatives if necessary.(2)
Know that “alternative medicine” treatments such as garlic or tea tree oil have not been proven to prevent your baby from becoming infected. Some treatments may be unsafe.
Wren’s mother followed an alternative regimen of acidophilus, echinacea, garlic capsules, vitamin C, grapefruit seed extract, and garlic suppositories to eradicate GBS from her body when pregnant with Wren. Wren was 7 pounds, 20.5 inches and perfect at birth after a normal labor and delivery at home. He died 11 hours later from a group B strep infection in his lungs.
Avoid unnecessary, frequent, or forceful internal exams which may push GBS closer to your baby. Knowing how far you are dilated does not accurately predict when your baby will be born.(8-10) Vaginal or perineal ultrasounds are less invasive options.(11,12)
Discuss the risks vs. benefits of possible methods of induction with your provider well before your due date as not all providers ask before “stripping” (also known as “sweeping”) membranes.
Ask your provider to not strip your membranes if you test positive for GBS. (Be aware that you may test negative, but be GBS+ later.) GBS can cross intact membranes and procedures such as stripping membranes and using cervical ripening gel to induce labor may push GBS as well as other bacteria closer to your baby.(13-16)
If you are having a planned C-section, talk to your provider about the potential risk of GBS infection and the risks vs. benefits of starting IV antibiotics for GBS well before your incision. IV antibiotics for GBS are not indicated per the US guidelines for a planned C-section done before your water breaks or labor starts as the risk of GBS infection in this situation is very low.
Talk to your provider about whether or not to use internal fetal monitors and/or have your water broken before you have had IV antibiotics for at least 4 hours.
Key Points
|
|
Call your healthcare provider. Report any fever. Remind them of your GBS status, including if GBS+ in a test done before 36 weeks. If you have previously had a baby with invasive GBS disease or have had GBS in your urine in this pregnancy, you should receive IV antibiotics regardless of this pregnancy’s GBS test result.
If you do not have a GBS test result at the onset of labor, IV antibiotics are indicated* for you per the US guidelines if you have any of the following risk factors:
Go to the hospital immediately if you should receive IV antibiotics. Have your GBS results with you. Be sure to tell the staff that you need to start IV antibiotics for GBS as soon as possible.
In half of GBS infections, the mother has no risk factors.(17) This is why testing is so important!
If you do not have a GBS test result at the onset of labor, IV antibiotics are indicated* for you per the US guidelines if you have any of the following risk factors:
- Your baby will be born before 37 weeks.
- Your water has been broken 18+ hours without delivering.
- You have a fever of 100.4°F (38°C) or higher during labor.
- Your test result from a rapid molecular test (if offered) is negative and any of the above risk factors develop.
- Your test result from a rapid molecular test (if offered) is positive.
- You were GBS positive in a previous pregnancy. *If this is your only risk factor and you are 37+ weeks, your healthcare provider may also choose to discuss IV antibiotics as an option.
Go to the hospital immediately if you should receive IV antibiotics. Have your GBS results with you. Be sure to tell the staff that you need to start IV antibiotics for GBS as soon as possible.
In half of GBS infections, the mother has no risk factors.(17) This is why testing is so important!
If you give birth before you have had 4 hours of antibiotics, the hospital may culture your baby and/or may observe him or her for 36–48 hours after birth.(18)
Be aware that your baby could still become infected even if you tested negative. Your baby could also become infected by other sources.
Breastfeeding can supply your baby with important antibodies to fight infection.(19) Although a few late-onset and recurrent GBS infections are possibly associated with infected breast milk, it is currently thought that the health benefits of breastfeeding outweigh any potential risk of exposure to GBS.(20-23)
Have everyone wash their hands before handling your baby.
Make sure everyone who takes care of your baby knows the signs of GBS infection in babies and how to respond.
Be aware that your baby could still become infected even if you tested negative. Your baby could also become infected by other sources.
Breastfeeding can supply your baby with important antibodies to fight infection.(19) Although a few late-onset and recurrent GBS infections are possibly associated with infected breast milk, it is currently thought that the health benefits of breastfeeding outweigh any potential risk of exposure to GBS.(20-23)
Have everyone wash their hands before handling your baby.
Make sure everyone who takes care of your baby knows the signs of GBS infection in babies and how to respond.
|
SIGNS OF GBS INFECTION IN BABIES |
Download our list of symptoms here to post for your family and your baby's caregivers
|
Call your baby’s care provider immediately or take your baby to the emergency room if you notice any of these signs:
- Sounds - High-pitched cry, shrill moaning, whimpering, inconsolable crying, constant grunting or moaning as if constipated or in distress
|
Crying sounds made by Wren who lived 11 hours due to GBS pneumonia
|
Grunting sounds made by Aayan who was diagnosed with GBS meningitis. The grunting sounds he made are a common, yet often unrecognized, symptom of GBS meningitis. Although Aayan was born premature, he was healthy except for apnea until he became infected by GBS at 98 days of age. He passed away 12 days later.
|
|
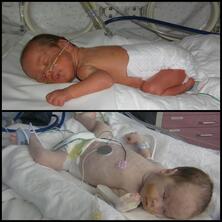
Above: Premature but otherwise healthy Jasmine
Below: Jasmine with cardiovascular shock-induced pallor due to late-onset GBS disease |
GBSI is a group of parents who are using their experiences with GBS to prevent heartache for other families. Please help us continue our efforts!
1. Savini V, et al. Streptococcus agalactiae vaginitis: nonhemolytic variant on the Liofilchem® Chromatic StreptoB. Int J Clin Exp Pathol. 2013; 6(8): 1693–1695.
2. American College of Obstetricians and Gynecologists Committee Opinion. Practice. Prevention of Early-onset Group B Streptococcal Disease in Newborns. ACOG Committee Opinion, Number 797, February 2020.
3. US. Preventive Services Task Force. Asymptomatic Bacteriuria in Adults: Screening. Sept. 24, 2019.
4. Cram L, Zapata M, Toy E, Baker III B. Genitourinary Infections and Their Association with Preterm Labor. Am Fam Physician. 2002;65(2):241-249.
5. Manning SD, Tallman P, Baker CJ, Gillespie B, Marrs CF, Foxman B. Determinants of co-colonization with group B streptococcus among heterosexual college couples. Epidemiology.2002 Sep;13(5):533-9.
6. Whitehead CL, Cohen N, Visser GHA, Farine D. Are increased fetal movements always reassuring? J Matern Fetal Neonatal Med. 2020 Nov;33(21):3713-3718.
7. Ostroff RM, Steaffans JW. Effect of specimen storage, antibiotics, and feminine hygiene products on the detection of group B Streptococcus by culture and the STREP B OIA test. Diagn Microbiol Infect Dis. 1995 Jul;22(3):253-9.
8. Imseis HM, Trout WC, Gabbe SG. The microbiologic effect of digital cervical examination. Am J Obstet Gynecol. 1999 Mar;180(3 Pt 1):578-80.
9. Soper DE, Mayhall CG, Froggatt JW. Characterization and control of intraamniotic infection in an urban teaching hospital. Am J Obstet Gynecol. 1996 Aug;175(2):304-9; discussion 309-10.
10. Weiss RE. Cervical Exam at the End of Pregnancy. www.verywellfamily.com. Updated June 14, 2021.
11. Lim BH. Transvaginal Ultrasound — Applications in the Second and Third Trimesters of Pregnancy. BMUS Bulletin. 2000;8(1):22-25.
12. Pan W, Chan L, Gau M. Accuracy of non-invasive methods for assessing the progress of labor in the first stage: a systematic review and meta-analysis. BMC Pregnancy Childbirth. 2022; 22: 608.
13. McGregor JA, Parsons A, French JI, Ultrasound Illustration of the Functional Connectedness of the Lower and Upper Reproductive Tracts. www.youtube.com
14. DeMott K., Cervical Manipulations linked to Perinatal Sepsis: Consider GBS-specific Chemoprophylaxis (Eight Case Reports). OB/GYN News, Oct. 15, 2001.
15. Sukumaran S, Chandraharan E. The Historical Practice of "Membrane Sweep" to Initiate Labour: Does it Have a Role in Contemporary Obstetric Practice? Glob J Reprod Med. 2021; 8(2): 5556733.
16. Hannah, Mary E. MD,CM, et. al. Maternal colonization with group B Streptococcus and prelabor rupture of membranes at term: the role of induction of labor. TermPROM Study Group. Am J Obstet Gynecol. 1997 Oct;177(4):780-5.
17. Rosenstein N, Schuchat A. Neonatal GBS Disease Study Group. Opportunities for prevention of perinatal group B streptococcal disease: A multistate surveillance analysis. Obstet Gynecol 90:901-6. 1997.
18. Puopolo KM, Lynfield R, Cummings J. Committee of Fetus and Newborn, Committee on Infectious Disease. Management of Infants at Risk for Group B Streptococcal Disease. Pediatrics, August 2019 Volume 144/Issue 2 from the American Academy of Pediatrics Clinical Report.
19. Lagergard T, Thiringer K, Wassen L, Schneerson R, Trollfors B. Isotype composition of antibodies to streptococcus group B type III polysaccharide and to tetanus toxoid in maternal, cord blood sera and in breast milk. Eur J Pediatr. 151(2):98-102. Feb 1992.
20. Lanari M, Serra L, Cavrini F, Liguori G, Sambri V , Late-onset group B streptococcal disease by infected mother’s milk detected by polymerase chain reaction. New Microbiol.2007 Jul;30(3):253-4.
21. Kotiw M, Zhang GW, Daggard G, Reiss-Levy E, Tapsall JW, Numa A. Late-onset and recurrent neonatal Group B streptococcal disease associated with breast-milk transmission. Pediatr Dev Pathol. 2003 May-Jun;6(3):251-6.
22. Sarasa NL, Mother’s Milk Still Best–and We Must Do Better. MEDICC Rev. 2013 Jan;15(1):48.
23. Meek JY, Noble L. American Academy of Pediatrics Policy Statement, Breastfeeding and the Use of Human Milk. Pediatrics (2022) 150 (1): e2022057988.
2. American College of Obstetricians and Gynecologists Committee Opinion. Practice. Prevention of Early-onset Group B Streptococcal Disease in Newborns. ACOG Committee Opinion, Number 797, February 2020.
3. US. Preventive Services Task Force. Asymptomatic Bacteriuria in Adults: Screening. Sept. 24, 2019.
4. Cram L, Zapata M, Toy E, Baker III B. Genitourinary Infections and Their Association with Preterm Labor. Am Fam Physician. 2002;65(2):241-249.
5. Manning SD, Tallman P, Baker CJ, Gillespie B, Marrs CF, Foxman B. Determinants of co-colonization with group B streptococcus among heterosexual college couples. Epidemiology.2002 Sep;13(5):533-9.
6. Whitehead CL, Cohen N, Visser GHA, Farine D. Are increased fetal movements always reassuring? J Matern Fetal Neonatal Med. 2020 Nov;33(21):3713-3718.
7. Ostroff RM, Steaffans JW. Effect of specimen storage, antibiotics, and feminine hygiene products on the detection of group B Streptococcus by culture and the STREP B OIA test. Diagn Microbiol Infect Dis. 1995 Jul;22(3):253-9.
8. Imseis HM, Trout WC, Gabbe SG. The microbiologic effect of digital cervical examination. Am J Obstet Gynecol. 1999 Mar;180(3 Pt 1):578-80.
9. Soper DE, Mayhall CG, Froggatt JW. Characterization and control of intraamniotic infection in an urban teaching hospital. Am J Obstet Gynecol. 1996 Aug;175(2):304-9; discussion 309-10.
10. Weiss RE. Cervical Exam at the End of Pregnancy. www.verywellfamily.com. Updated June 14, 2021.
11. Lim BH. Transvaginal Ultrasound — Applications in the Second and Third Trimesters of Pregnancy. BMUS Bulletin. 2000;8(1):22-25.
12. Pan W, Chan L, Gau M. Accuracy of non-invasive methods for assessing the progress of labor in the first stage: a systematic review and meta-analysis. BMC Pregnancy Childbirth. 2022; 22: 608.
13. McGregor JA, Parsons A, French JI, Ultrasound Illustration of the Functional Connectedness of the Lower and Upper Reproductive Tracts. www.youtube.com
14. DeMott K., Cervical Manipulations linked to Perinatal Sepsis: Consider GBS-specific Chemoprophylaxis (Eight Case Reports). OB/GYN News, Oct. 15, 2001.
15. Sukumaran S, Chandraharan E. The Historical Practice of "Membrane Sweep" to Initiate Labour: Does it Have a Role in Contemporary Obstetric Practice? Glob J Reprod Med. 2021; 8(2): 5556733.
16. Hannah, Mary E. MD,CM, et. al. Maternal colonization with group B Streptococcus and prelabor rupture of membranes at term: the role of induction of labor. TermPROM Study Group. Am J Obstet Gynecol. 1997 Oct;177(4):780-5.
17. Rosenstein N, Schuchat A. Neonatal GBS Disease Study Group. Opportunities for prevention of perinatal group B streptococcal disease: A multistate surveillance analysis. Obstet Gynecol 90:901-6. 1997.
18. Puopolo KM, Lynfield R, Cummings J. Committee of Fetus and Newborn, Committee on Infectious Disease. Management of Infants at Risk for Group B Streptococcal Disease. Pediatrics, August 2019 Volume 144/Issue 2 from the American Academy of Pediatrics Clinical Report.
19. Lagergard T, Thiringer K, Wassen L, Schneerson R, Trollfors B. Isotype composition of antibodies to streptococcus group B type III polysaccharide and to tetanus toxoid in maternal, cord blood sera and in breast milk. Eur J Pediatr. 151(2):98-102. Feb 1992.
20. Lanari M, Serra L, Cavrini F, Liguori G, Sambri V , Late-onset group B streptococcal disease by infected mother’s milk detected by polymerase chain reaction. New Microbiol.2007 Jul;30(3):253-4.
21. Kotiw M, Zhang GW, Daggard G, Reiss-Levy E, Tapsall JW, Numa A. Late-onset and recurrent neonatal Group B streptococcal disease associated with breast-milk transmission. Pediatr Dev Pathol. 2003 May-Jun;6(3):251-6.
22. Sarasa NL, Mother’s Milk Still Best–and We Must Do Better. MEDICC Rev. 2013 Jan;15(1):48.
23. Meek JY, Noble L. American Academy of Pediatrics Policy Statement, Breastfeeding and the Use of Human Milk. Pediatrics (2022) 150 (1): e2022057988.
Join the Campaign against GBS Disease in babies! |
CONNECT TO GBSI |