What is early-onset group B strep disease?
Group B Strep infections which occur within the first week of life are called “early-onset” GBS disease. It is currently the only type of GBS disease that has a recommended prevention strategy. Many countries recommend that all pregnant individuals should be screened for GBS (“universal screening”) and, if positive, given IV antibiotics during labor and delivery to help prevent early-onset GBS disease. Early-onset infections are typically acquired vertically through exposure to GBS from the vagina of a colonized birthing parent, although the baby may become infected from sources other than the birthing parent after birth.
“Prevention is better than cure.” – Desiderius Erasmus
How to Help Prevent Early-onset Group B Strep
Ideally, your healthcare provider should do a urine culture for GBS and other bacteria at the first prenatal visit. GBS in your urine means that you are likely heavily colonized vaginally. If your urine tests positive, your provider should consider you as “GBS colonized” for this pregnancy.
It is now the standard of care in the USA for all pregnant individuals to be routinely tested for GBS with a vaginal/rectal swab test during the 36th or 37th week during each pregnancy unless their urine already cultured positive in the current pregnancy or they have had a previous baby with GBS disease. The swab test is a culture of a swab that has been inserted in both the vagina and rectum. Inform your healthcare provider if you are using antibiotics and/or vaginal medications which may cause false negative results. GBS is a transient bacteria which means that a person could test negative, but be colonized later in pregnancy and vice versa, but the results are considered to accurately (95%-98%) predict a pregnant individuals colonization status at delivery if she delivers within 5 weeks of her test.
However, studies have found that even in the era of universal screening, >60% of early-onset GBS cases have occurred among infants born to a parent who had a negative prenatal GBS culture screen - this is why everyone should be aware of the signs of GBS.
It is now the standard of care in the USA for all pregnant individuals to be routinely tested for GBS with a vaginal/rectal swab test during the 36th or 37th week during each pregnancy unless their urine already cultured positive in the current pregnancy or they have had a previous baby with GBS disease. The swab test is a culture of a swab that has been inserted in both the vagina and rectum. Inform your healthcare provider if you are using antibiotics and/or vaginal medications which may cause false negative results. GBS is a transient bacteria which means that a person could test negative, but be colonized later in pregnancy and vice versa, but the results are considered to accurately (95%-98%) predict a pregnant individuals colonization status at delivery if she delivers within 5 weeks of her test.
However, studies have found that even in the era of universal screening, >60% of early-onset GBS cases have occurred among infants born to a parent who had a negative prenatal GBS culture screen - this is why everyone should be aware of the signs of GBS.
If your urine or swab tests are positive or you have had a previous baby with GBS disease, your provider should consider you as “GBS colonized” for this pregnancy so that you receive IV antibiotics for GBS when labor starts or your water breaks. Plan ahead if you have short labors or live far from the hospital. The IV antibiotics you receive in labor generally take 4 hours to be optimally effective.
C-sections may not completely prevent iGBS infection although, according to ACOG, the risk of early-onset infection for a full term baby during a planned C-section is extremely low if performed before your labor starts and before your water breaks. According to the current ACOG guidelines in the US, pregnant individuals with a positive prenatal GBS culture result who undergo a cesarean birth before the onset of labor and with intact membranes do not require GBS antibiotic prophylaxis.
If you do not have a GBS test result, and your hospital does not offer a rapid GBS test, per the ACOG guidelines you should be offered IV antibiotics based on the following risk factors:
C-sections may not completely prevent iGBS infection although, according to ACOG, the risk of early-onset infection for a full term baby during a planned C-section is extremely low if performed before your labor starts and before your water breaks. According to the current ACOG guidelines in the US, pregnant individuals with a positive prenatal GBS culture result who undergo a cesarean birth before the onset of labor and with intact membranes do not require GBS antibiotic prophylaxis.
If you do not have a GBS test result, and your hospital does not offer a rapid GBS test, per the ACOG guidelines you should be offered IV antibiotics based on the following risk factors:
- Your baby will be born before 37 weeks.
- Your water has been broken 18+ hours without delivering.
- You have a fever of 100.4 °F or higher during labor.
- Intrapartum NAAT result is negative but above risk factors develop
- Intrapartum NAAT result positive for GBS
- You were GBS colonized in a previous pregnancy.
What are the odds of a baby developing early-onset GBS disease
if the pregnant parent tests positive for GBS?
if the pregnant parent tests positive for GBS?
If the pregnant individual receives IV antibiotics during labor and delivery, there is only a 1 in 4,000 chance of delivering a baby who will develop early-onset GBS disease. However, if the pregnant individuals does NOT receive IV antibiotics during labor and delivery, the likelihood of their baby developing early-onset GBS disease jumps to just 1 in 200.
The Signs of Early-onset Group B Strep
|
Even if parents has taken all the offered steps to prevent group B strep, there is still a possibility of an invasive group B strep infection in her baby. After birth a baby can become infected from sources other than the birthing parent and >60% of early-onset cases occur to infants whose birthing parent tested negative.
This is why knowing and recognizing the signs is so important! GBS is a fast-acting type of bacteria, potentially making an otherwise healthy-appearing baby critically ill within hours. Being able to recognize the signs of infection is imperative for seeking and receiving prompt medical treatments for better outcomes. Help make sure no baby is overlooked! |
Once your baby is born, if any of these signs are recognized, contact your care provider immediately:
- Temperature: fever, low or unstable temperature
- Eating habits: feeds poorly, refuses to eat, not waking to feed, vomiting
- Sleeping habits: sleeping too much, difficulty being aroused
- Breathing: fast, slow or difficult breathing
- Sounds: high pitch cry, shrill moaning, whimpering, inconsolable, constant grunting
- Behavior: marked irritability, reacting as if skin is tender, listless, floppy, not moving an arm or leg, blank stare, body stiffening, uncontrollable jerking
- Skin Appearance: blue, gray or pale skin, blotchy or red skin, tense or bulgy fontanel, infection at the base of umbilical cord or head punctures from internal fetal monitor
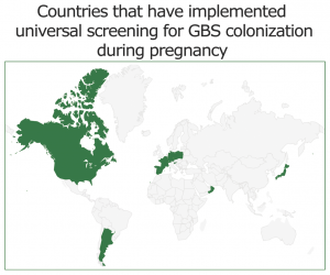
Early-onset Prevention Worldwide
|
Countries that have implemented universal screening for GBS colonization during pregnancy include Canada, United States of America, Argentina, Spain, France, Belgium, Germany, Switzerland, Czech Republic, Poland, Slovenia, Hong Kong, and Japan as well as regions of Italy and Australia.
Efforts are being made worldwide to implement better GBS care in all countries. Please share country-focused resources and articles with GBSI at [email protected]. |
Join the Campaign against GBS Disease in babies! |
CONNECT TO GBSI |